Microsporidiosis is an opportunistic intestinal infection that causes diarrhea and wasting in immunocompromised individuals (HIV, for example). It results from different species of microsporidia, a group of microbial (unicellular) fungi.
In HIV infected individuals, microsporidiosis generally occurs when CD4+ T cell counts fall below 150.
Classification

Although it is classified as a protozoal disease in ICD-10, their phylogenetic placement has been resolved to be within the Fungi; however, they are highly divergent and rapidly evolving. As unicellular eukaryotes they are still generally considered to be Protists, and some sources classify microsporidiosis as a mycosis.
Causative agents
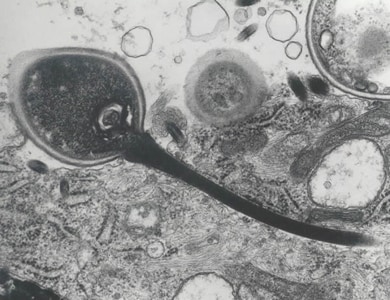
At least 14 microsporidian species have been recognized as human pathogens, spread across eight genera:
- Brachiola
- B. algerae, B. connori, B. vesicularum
- Encephalitozoon
- E. cuniculi, E. hellem, E. intestinalis
- Enterocytozoon
- E. bieneusi
- Microsporidium
- M. ceylonensis, M. africanum
- Nosema
- N. ocularum
- Pleistophora sp.
- Trachipleistophora
- T. hominis, T. anthropophthera
- Vittaforma
- V. corneae.
The primary causes are Enterocytozoon bieneusi and Encephalitozoon intestinalis.
Life cycle

(Coded to image at right).
- The infective form of microsporidia is the resistant spore and it can survive for an exteneded period of time in the environment.
- The spore extrudes its polar tubule and infects the host cell.
- The spore injects the infective sporoplasm into the eukaryotic host cell through the polar tubule.
- Inside the cell, the sporoplasm undergoes extensive multiplication either by merogony (binary fission) or schizogony (multiple fission).
- This development can occur either in direct contact with the host cell cytoplasm (E. bieneusi) or inside a vacuole called a parasitophorous vacuole (E. intestinalis). Either free in the cytoplasm or inside a parasitophorous vacuole, microsporidia develop by sporogony to mature spores.
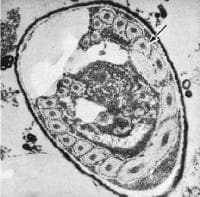
- During sporogony, a thick wall is formed around the spore, which provides resistance to adverse environmental conditions. When the spores increase in number and completely fill the host cell cytoplasm, the cell membrane is disrupted and releases the spores to the surroundings.
- These free mature spores can infect new cells thus continuing the cycle.
Treatment
Fumagillin has been used in the treatment.
Another agent used is albendazole.
References

External links

- CDC's microsporidiosis info page.







0 comments:
Post a Comment